Learn how remote patient monitoring (RPM) programs work, their reimbursement structure, and how health systems use RPM to improve outcomes and reduce costs.
Health systems managing large chronic patient populations face increasing pressure to improve outcomes while controlling costs. Rising readmission penalties, workforce shortages, and the shift toward value-based care models are forcing organizations to rethink how care is delivered beyond hospital walls.
Remote Patient Monitoring (RPM) has emerged as a key strategy to address these challenges. By enabling clinicians to track patient vitals and health data in real time from home, RPM allows health systems to detect complications earlier, intervene sooner, and reduce avoidable hospital utilization.
For organizations participating in value-based contracts, RPM also provides a scalable mechanism to improve chronic disease outcomes while generating structured reimbursement through Medicare’s RPM billing framework.
What Remote Patient Monitoring Offerings Include
Modern RPM programs combine connected devices, digital platforms, and clinical monitoring workflows to ensure continuous patient oversight.
Typical RPM offerings include:
- Connected medical devices such as blood pressure monitors, glucose meters, weight scales, and pulse oximeters
- Automated data transmission through cellular or Bluetooth-enabled devices
- Clinical monitoring platforms that aggregate patient readings and trigger alerts for abnormal values
- Care management teams responsible for reviewing data and contacting patients when intervention is required
- Documentation and compliance workflows aligned with CMS RPM billing requirements
Together, these components create a structured monitoring ecosystem that extends care beyond traditional clinical visits.
How RPM Programs Work: Operational Workflow
A typical RPM program follows a structured process designed to support continuous patient engagement and clinical oversight.
1. Patient Identification and Enrollment
Health systems begin by identifying patients who would benefit most from continuous monitoring, typically those with chronic conditions or high readmission risk.
- Risk-based patient selection: Patients with hypertension, diabetes, heart failure, or COPD are prioritized.
- Program enrollment: Eligible patients are onboarded into the RPM program during clinic visits or post-discharge transitions.
- Device provisioning: Patients receive connected devices along with instructions for home use.
2. Daily Health Data Collection
Patients capture vital signs from home using connected devices, enabling consistent monitoring without requiring frequent clinic visits.
- Routine vital measurements: Blood pressure, glucose, oxygen saturation, heart rate, or weight.
- Automatic data transmission: Cellular or Bluetooth devices send readings directly to the monitoring platform.
- Reliable data capture: Eliminates manual reporting and reduces documentation errors.
3. Intelligent Monitoring and Alerts
RPM platforms organize incoming data and highlight patients who require immediate attention, helping care teams manage large populations efficiently.
- Centralized dashboards: Clinicians view patient data trends across the monitored population.
- Threshold-based alerts: Systems flag abnormal readings that fall outside clinical parameters.
- Prioritized patient review: Care teams focus on patients most likely to require intervention.
4. Proactive Patient Outreach
When abnormal readings occur, care teams contact patients to evaluate symptoms and prevent complications.
- Clinical follow-up: Nurses or care coordinators reach out to assess the patient's condition.
- Care plan adjustments: Medication guidance, lifestyle recommendations, or physician consultations may follow.
- Escalation protocols: Patients showing concerning trends may be scheduled for in-person visits.
5. Continuous Care Optimization
Over time, RPM data provides deeper insight into patient health patterns and treatment effectiveness.
- Trend-based treatment adjustments: Clinicians refine medications or therapies based on long-term readings.
- Improved patient adherence: Regular monitoring encourages patients to stay engaged in their care plans.
- Population health insights: Aggregated data helps health systems identify high-risk groups and optimize care strategies.
Financial Impact of RPM for Health Systems
For economic decision-makers, RPM’s value extends beyond clinical benefits. When implemented at scale, RPM can produce a measurable financial impact.
Reduced Hospital Utilization
Continuous monitoring allows clinicians to detect early signs of deterioration, preventing complications that often lead to emergency department visits or hospital admissions.
Improved Performance in Value-Based Programs
RPM supports better chronic disease management and utilization metrics, helping organizations perform more effectively in value-based contracts and bundled payment programs.
New Reimbursement Opportunities
Medicare reimburses RPM services through several CPT codes, allowing providers to generate recurring revenue while delivering proactive care.
Staffing Efficiency
Structured RPM programs allow centralized monitoring teams to oversee large patient populations, reducing the need for reactive, labor-intensive care management.
For health systems managing thousands of chronic patients, these factors collectively create meaningful improvements in cost control and operational efficiency.
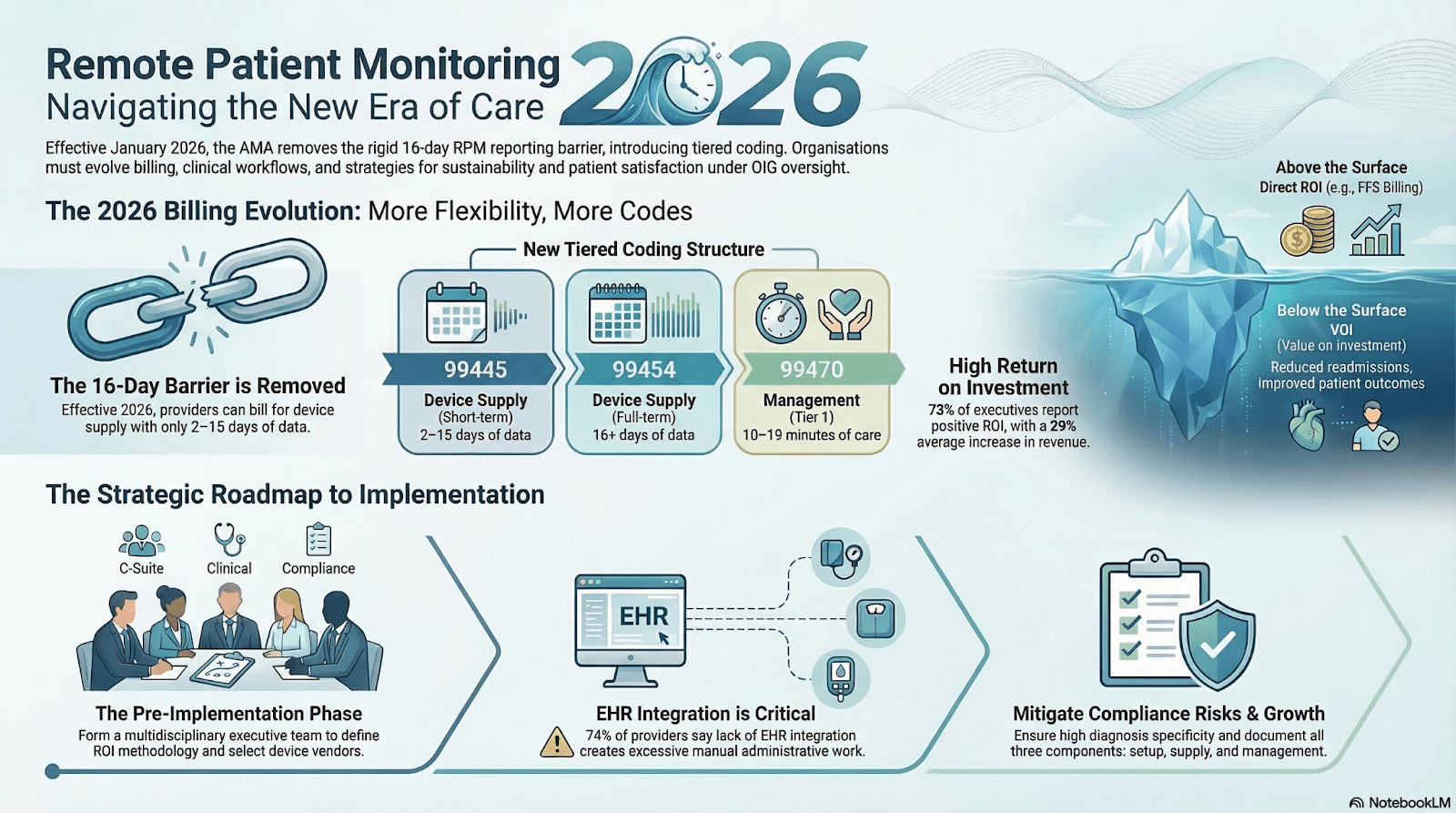
Key CMS Billing Codes Supporting RPM Programs
Medicare provides reimbursement for RPM services through several CPT codes:
Proper documentation, consistent device usage, and structured monitoring workflows are essential for maintaining compliance and maximizing reimbursement.
Clinical Outcomes Associated With Remote Patient Monitoring
Remote patient monitoring programs deliver measurable improvements in both clinical outcomes and care coordination. By providing continuous visibility into patient health between visits, RPM enables earlier interventions and more consistent chronic disease management.
Better Control of Chronic Conditions
Continuous monitoring helps clinicians detect trends earlier and adjust treatments before complications occur.
- Hypertension management: Regular blood pressure monitoring enables timely medication adjustments.
- Diabetes monitoring: Frequent glucose tracking supports better glycemic control.
- Heart failure management: Daily weight and symptom monitoring help identify fluid retention before it escalates.
Earlier Detection of Patient Deterioration
RPM provides real-time insight into patient health changes, allowing providers to respond faster than traditional care models.
- Alert-based monitoring: Abnormal readings trigger alerts for clinical review.
- Timely intervention: Care teams can contact patients before symptoms worsen.
- Preventive escalation: Patients can be directed to outpatient care instead of emergency departments.
Reduced Hospitalizations and Readmissions
By addressing health risks early, RPM helps prevent avoidable hospital utilization.
- Post-discharge monitoring: Patients recently discharged from hospitals receive closer oversight.
- Complication prevention: Early outreach prevents conditions from escalating into acute events.
- Lower readmission risk: Continuous monitoring supports smoother recovery during vulnerable transition periods.
Higher Patient Engagement and Treatment Adherence
Regular monitoring encourages patients to stay actively involved in their health management.
- Daily health awareness: Patients better understand how behaviors affect their conditions.
- Improved medication adherence: Care teams can reinforce treatment plans during outreach.
- Stronger patient-provider connection: Ongoing engagement builds trust and accountability.
Improved Care Coordination Across Teams
RPM data provides clinicians with a consistent view of patient health across care settings.
- Shared clinical insights: Providers can review patient trends between visits.
- More informed decision-making: Treatment plans are based on continuous health data rather than episodic snapshots.
- Better population health oversight: Care teams can identify high-risk patients earlier.
Why Many Health Systems Struggle to Scale RPM Internally
Despite its benefits, implementing RPM at scale presents operational challenges.
Common barriers include:
- Managing high volumes of incoming patient data
- Maintaining consistent monitoring and outreach workflows
- Ensuring CMS-compliant documentation for billing
- Integrating RPM data with existing clinical systems
- Staffing clinical teams to manage patient engagement
Without the right infrastructure, RPM programs can become difficult to sustain and scale.
Scaling Remote Patient Monitoring With Circle Care Health
To overcome these challenges, many health systems partner with specialized care management providers.
Circle Care Health supports RPM implementation through an integrated model that combines:
- AI-enabled monitoring platforms
- Connected device infrastructure
- Dedicated clinical care teams
- Structured outreach workflows
- CMS-compliant documentation and reporting
This approach enables health systems to deploy RPM programs quickly while minimizing operational burden and ensuring consistent patient engagement.
The Growing Role of RPM in Value-Based Care
As healthcare continues shifting toward value-based reimbursement, proactive monitoring models like RPM are becoming increasingly important.
Health systems that successfully integrate remote monitoring can:
- Improve chronic disease outcomes
- Reduce preventable utilization
- Strengthen performance in risk-based contracts
- Maintain continuous engagement with high-risk patients
RPM transforms episodic care into a continuous care model, one that better aligns with the goals of modern healthcare delivery.
Conclusion
Remote Patient Monitoring is rapidly becoming a core capability for health systems seeking to manage chronic populations more effectively. By enabling continuous patient oversight and earlier clinical intervention, RPM programs improve outcomes while reducing avoidable utilization.
However, scaling these programs requires the right combination of technology, clinical workflows, and operational support. Health systems that partner with experienced care management providers can implement RPM more efficiently and unlock its full clinical and financial potential.
See how Circle Health Care helps health systems scale remote patient monitoring programs without increasing operational burden. Schedule a demo to explore how our RPM solutions support better outcomes and sustainable growth.